1. In-vitro fertilisation techniques |
2. IVF protocols |
3. The efficiency of IVF methods |
4. Secrets of successful IVF |
5. IVF clinics abroad |
Having a child is possible practically for anyone regardless of their reproductive status thanks to modern medicine. The average success rate of IVF abroad is 55-65%, and in some cases, it can be as high as 80%!
There are many methods of artificial insemination. In this article, we explain in detail the advantages and indications of the different methods, what percentage of effectiveness you should expect and which foreign clinics to contact.
Listen to the article:
Artificial insemination is a reproductive medicine method that allows patients with fertility problems to achieve pregnancy. Sometimes it is also used by single people who want to have a new addition to their family.
In in vitro fertilisation (IVF), mature eggs and sperm are taken from patients (or donors) and fertilised in a laboratory. After a few days, the formed embryo is transferred to the uterus.
Artificial insemination methods
ICSI
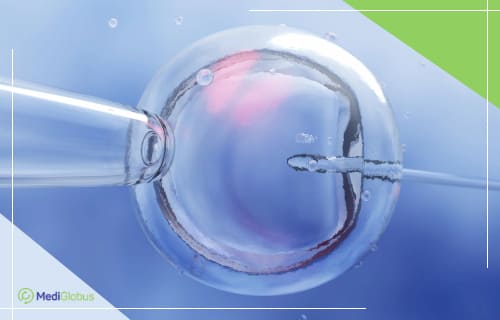
Unlike conventional IVF, intracytoplasmic sperm injection (ICSI) involves a doctor manually inserting the sperm into the egg to fertilise it. This method is used in about 70% of all IVF procedures.
Indications for ICSI:
Male infertility (low sperm count, low mobility or abnormal sperm shape);
Conducting testicular sperm extraction (TESE);
Failure of a conventional IVF treatment;
In Vitro Maturation of Oocytes (IVM);
Use of frozen oocytes;
In preimplantation genetic testing (PGT).
On average 50-80% of eggs are fertilised after ICSI, whereas with conventional IVF the rate is 50%. Once the embryo has formed, the success rate is the same as for the standard procedure.
Since ICSI is most often performed in cases where the sperm is of poor quality, one should keep in mind the fact that this group of patients has a higher risk of transmitting genetic diseases to the child. Genetic analysis of the foetus is therefore recommended.
There is also a variation of this method called IMSI (intracytoplasmic injection of morphologically selected spermatozoa). Its key difference is that IMSI uses a powerful microscope to select the best sperm.
IVF in the natural cycle
IVF in a natural cycle eliminates the ovarian stimulation step used to produce multiple mature oocytes. In standard IVF, this increases the chance of a successful outcome, since with more eggs there is a higher chance that one of them will form a healthy embryo and implant in the uterus. However, for some women, high doses of hormones required for ovarian stimulation can be unpleasant or harmful. Even for healthy patients, the procedure is very stressful on the body, so there is always a minimum of a month’s rest and recovery between IVF attempts.
IVF in the natural cycle is recommended for patients with low ovarian reserve.
For IVF in the natural cycle, patients still need injections of hormones, but in much smaller doses. They are administered to prevent early ovulation and support normal oocyte growth.

On average, 14 mature oocytes can be extracted in one cycle in a woman under 35 years of age. In 40-year-olds, only 8 can be obtained with the same protocol.
The advantage of IVF in a natural cycle is the high quality of the eggs, less stress for the body and the possibility to have several attempts of artificial insemination in a row.
Because there is no cost for additional medication, the price for IVF in a natural cycle is usually lower than a standard procedure.
Before an oocyte retrieval, women have regular ultrasound scans of their ovaries and necessary blood tests. The oocyte is taken from the dominant ovary when it has reached the required size.
Appointment for an IVF
Foreign fertility centres offer a wide range of IVF plans. To book an appointment with an experienced reproductive therapist, please leave your request on our website.
Japanese IVF protocol
IVF with minimal stimulation, also known as the Japanese protocol, is a compromise between the standard IVF protocol and IVF in the natural cycle:
Mini-IVF is designed to collect just a few high-quality eggs, allowing to:
Avoid the risk of ovarian hyperstimulation syndrome;
Reduce the cost of medication by up to 10 times;
Reduce the number of injections;
Avoid painful progesterone injections.
For older women, the Japanese IVF protocol offers the same number of healthy eggs as the conventional procedure, but with less discomfort and lower cost of medication.
With mini-IVF, just like with IVF in the natural cycle, there is a lower chance of twins or triplets being born.
IVF with donor sperm/egg
IVF with donor sperm or eggs is used if:
Low quality of patient’s sperm or eggs;
The patient does not have a partner;
Both partners are of the same sex.
In general terms, the IVF procedure with donor material is the same as for other protocols. In IVF with a donor egg, you will need to wait for the menstrual cycles of the donor and the recipient to synchronise – otherwise, embryo transfer wouldn’t be possible. This can take several months, but usually no more than two or three.
If a woman wants to undergo IVF without her husband, fertility clinics send a request to a sperm bank. These organisations select a donor based on the criteria provided by the patient. Usually, the sperm donors are anonymous, but IVF applicants can still find out basic information about them that may influence their future child: weight, height, skin, eye and hair colour, and IQ level.
IVF with a donor egg and donor sperm is also possible.
For same-sex couples, there is the option of reciprocal IVF. This is a procedure with donor sperm in which the partners are reciprocally implanted with embryos derived from each other’s eggs. This allows both mothers to take part in the formation of the child.
The selection protocol for both egg donors and sperm donors is quite strict. Only people aged 18-39 (up to 35 for women) in good health without any genetic abnormalities and with quality gametes are accepted for this role. For couples, it is possible to find a donor similar to the husband, so that the child also resembles the father.
It is important for medical tourists to bear in mind that the laws regarding reproductive medicine may differ abroad. Many IVF clinics have lawyers to advise prospective parents on the legal side of the issue.

Cryopreserved embryo transfer (FET, GIFT, eSET)
FET is a standard procedure in which embryos are frozen after they have been obtained. This is done to avoid having to transfer several embryos, which can lead to a riskier twin or triplet pregnancy. The frozen embryos can be used in subsequent menstrual cycles.
In eSET, only one embryo is transplanted, individually selected by the reproductive surgeon based on several criteria – size and number of cells, stage of development, etc. The procedure is performed if the parents want to avoid multiple pregnancies – the chance of twins being born with this method is only 1-2%.
GIFT (gamete intrafallopian transfer) is an assisted IVF method in which fertilisation takes place inside the mother’s body. For this, the zygote is placed in the fallopian tube within 24 hours of the doctor ‘mixing’ the egg with the sperm. The method is used if the traditional IVF protocol, in which the embryo is transferred on days 3 to 5, does not produce the expected results.
IVF protocols
IVF protocols are different combinations of medical products that are used to obtain mature eggs. A fertility doctor selects the most relevant one depending on the age and reproductive health of the patient, as well as her individual preferences.
During the menstrual cycle, the woman is closely monitored by a doctor, who will conduct regular ultrasound examinations and blood tests. If necessary, the dosage of the medications will be adjusted.
Regardless of the chosen IVF protocol, it is usually recommended to take the oral contraceptive prescribed by your doctor for a few days or weeks before starting ovarian stimulation to regulate your menstrual cycle.
IVF protocol with antagonists
In the IVF protocol with antagonists, patients start taking gonadotropins – hormones that stimulate egg production – at the beginning of the menstrual cycle. After 4-6 days, a GnRH antagonist injection is given to prevent all follicles from ovulating. By days 8-12, the follicles will have reached the correct size. Then an injection of a GnRH agonist hormone or hCG is given and the eggs are retrieved within the next 36 hours.
This protocol is considered to be the most universal. It is suitable for women at high risk of developing ovarian hyperstimulation syndrome.
Long IVF protocol
For a long IVF protocol, patients start using GnRH agonists about a week before the start of their menstrual cycle. After that, the protocol continues similarly to the previous one, but with lower doses of the hormone in question.
A long IVF protocol is used to avoid premature ovulation – when the eggs move into the fallopian tube.
Short IVF protocol
The short IVF protocol uses the same drugs as the long protocol. The difference is that the GnRH agonist is administered at a lower dose and that it is started on the first day of the cycle. Then, after 1-2 days of the same cycle, gonadotropins are administered to the woman.
This protocol is recommended for patients with a low oocyte reserve or with previous IVF failures. However, it is used with caution in women at high risk of ovarian hyperstimulation syndrome.
After a positive pregnancy test, you will need to take medication to support the function of the corpus luteum for 3-6 weeks. This will help keep the pregnancy safe until the placenta develops.
The effectiveness of IVF methods
Calculating the effectiveness of artificial insemination is difficult, as a large number of factors play a role.
IVF statistics in different reproductive clinics can vary considerably, being higher or lower than those presented by medical communities. This is because physicians take proprietary approaches in preparing embryos and patients for pregnancy. This factor should be taken into account when choosing the clinic where the planned procedure will take place.
The biggest factor affecting the chances of getting pregnant is the age of the mother. According to the Society of Assisted Reproductive Technology (SART), the average IVF success rate by age, without considering the treatment method, is as follows:
| Age | Effectiveness of IVF |
|---|---|
| Under 35 years | 55,6% |
| 35-37 years old | 40,8% |
| 38-40 years old | 26,8% |
| 41-42 years old | 12,6% |
| +43 years old | 3,9% |
Despite the statistics, one should not assume that age rules out the possibility of becoming a mother through IVF. Firstly, there are methods to increase the likelihood of pregnancy, such as assisted hatching and uterine endometrial scraping. Secondly, even if age becomes a barrier, surrogacy remains an option. If the patient still has healthy eggs, these can be fertilised and transplanted to a younger woman who will bear a child.
In addition, it should be remembered that the cause of infertility plays a major role. For example, the success rate of IVF in stage 3-4 endometriosis is reduced in comparison to healthy women or patients with stage 1-2 disease. Despite this, in-vitro fertilisation remains the recommended method of pregnancy with this diagnosis. Performing surgery to treat endometriosis can significantly improve the chances of successful IVF.
The secrets of successful IVF
Although some of the factors that influence IVF success are beyond patients’ control, there are still things that can be influenced.
Choose the right centre for reproductive medicine
IVF success rates vary considerably from one centre to another. When choosing a hospital, you should thoroughly research all available options, not only in terms of the cost of procedures but also statistics on the effectiveness of the treatment, the available assistive methods, the certification and experience of the doctor, etc. MediGlobus coordinating physicians can help you quickly sort this out and advise you on the best IVF clinic abroad based on your budget.
Careful diagnosis of both partners
To choose the right IVF method, it is important to understand exactly why you are having difficulty getting pregnant. Even if you know for sure that the problem is with one partner – for example, the woman cannot get pregnant after cancer treatment – you should still carry out a reproductive diagnosis of the husband.
Changing the diet
A study by the Harvard School of Public Health has shown that eating foods rich in monounsaturated fats increase fertility. These include avocados, nuts and seeds, sunflower oil and olive oil. Apart from increasing the chances of getting pregnant, fats are also essential for the development of the foetus. Low glycaemic index foods, alcohol and caffeine should also be avoided. Both partners should quit smoking, as nicotine significantly reduces sperm quality and the success of IVF.
Avoiding stress
Stress hormones hurt a woman’s ability to get pregnant, so you should try to eliminate all factors that cause anxiety during treatment. Of course, all patients are anxious about IVF, but dealing with emotions can be done in different ways. Many fertility centres offer couples the opportunity to consult a psychologist. This will not only provide an opportunity to develop stress management skills but also discuss specific issues and anxieties common to parents resorting to IVF. Yoga and meditation can be useful habits to get into. They have been proven to reduce the levels of stress hormones in the blood, and shared activities will help to bring the couple closer together on their journey to starting a family.
Medication therapy
Experienced reproductive therapists can prescribe vitamins and supplements to improve the quality of eggs and sperm.
Complementary treatment
Based on the diagnostic findings, an experienced reproductive therapist can recommend specific treatments that will increase the chance of successful IVF. Such recommendations are strictly individualised. These include, for example, blastocyst culture, assisted hatching (LAH), uterine endometrial scraping, surgical treatment of endometriosis, etc;
IVF clinics abroad
Resume
IVF is a group of reproductive medicine methods used to help people suffering from infertility. The methods are based on the artificial insemination of an egg ‘in a tube’, after which the resulting zygote is transferred to the woman.
There are different types of IVF: IVF with ICSI, IVF in the natural cycle, IVF with donor sperm and/or eggs, and cryopreserved embryo transfer. Depending on the causes of infertility, an experienced reproductive surgeon will help you choose the most effective option.
IVF protocols are a plan for taking medication to prepare the woman for egg retrieval. Antagonist IVF protocols are standard, but there are also short and long IVF protocols, and mini-EVF (Japanese protocol). Their choice depends on the age of the patient, the available oocyte reserve, the risk of ovarian hyperstimulation syndrome and other factors.
The age of the patient and the cause of infertility have the most influence on the effectiveness of IVF, but other factors also play a role. The success of in-vitro fertilisation may vary considerably from clinic to clinic, so you should carefully consider your options before making your choice.
In addition to biological factors, lifestyle-related factors also influence the success of IVF. Adjusting your diet, and avoiding bad habits and stress can increase your chances of a successful outcome.
The international MediGlobus platform offers free help in choosing a fertility centre. Leave your request on our website and we will call you back within a few hours to answer all your questions and give you the best consultation according to your criteria.
Sources:
- 1. Statistics from the Society for Assisted Reproductive Technology
- 2. Harvard research on the relationship between diet and fertility











