Modern women are taking their health more seriously from a young age. But the question remains – among many methods of diagnosis, which one is the most accurate? To understand this topic better, read our article.
Listen to the article:
What methods are available for diagnosing breast cancer?
The main methods doctors use to diagnose breast tumours include:
Mammography;
3D mammography;
Breast ultrasound;
Contrast-enhanced mammography (CEM);
Breast MRI;
Scintigraphy;
Positron emission mammography (PET);
Elastography.

The methods are not interchangeable and are used in different situations – depending on the patient’s risk group, breast tissue density, results of other tests and other factors. In many cases, it is possible to discover if the neoplasm is benign or not. 90% of tumours detected in the breast are not cancerous.
Otherwise, if the scans show signs of a malignant process, doctors will prescribe a biopsy. This is a medical procedure where a small sample of tissue from the tumour is taken with a needle and analysed in a laboratory. It is the only way to confirm a diagnosis of cancer.
Breast cancer detected at an early stage is easier to treat successfully. According to the WHO, the American Cancer Society and other organisations, having regular screening tests is the surest way to detect breast cancer at an early stage. These patients are less likely to need aggressive treatment, such as breast surgery and chemotherapy, and are more likely to achieve complete remission.
There are international guidelines that determine how often women should have breast screening. They take into account two main factors: age and the presence of genetic risk. The latter includes having female relatives who have had cancer, the presence of a BRCA mutation, or having been exposed to high doses of radiation.
Women 40-44 years old at medium risk | Women 45-54 years old with medium risk | Women aged 55+ years with intermediate risk | Women 30+ years at high risk |
|---|---|---|---|
| Depending on doctor’s recommendation may need to start having an annual check-up | Have an annual check-up | Depending on doctor’s recommendation, continue to have a check-up every 1-2 years | An in-depth check-up every year |
Book an appointment for breast screening
Leave an enquiry online and we’ll help you find a cost-effective package for your annual breast screening at a top-level certified clinic.
Method 1. Breast self examination
One of the most popular and readily available methods of checking your breasts is a self examination. It is recommended that you have one every month.
However, as of 2019, the American Association of Oncologists does not recommend this method of diagnosis for women who are not at high risk. After analysing data from several countries, they found that self-examination does not help to detect breast cancer more often.
At the same time, for women at higher risk of developing breast cancer, self-examination can remain a useful habit if it is combined with regular examinations by a mammalogist and imaging diagnostics.
To check your breasts yourself, follow these steps:
Stretch your shoulders, put your hands on your hips and examine your breasts in a mirror. Look for any unusual changes – nipple shape and size, rashes or skin thickening.
Examine your breasts by raising your hands up and bringing them together above your head.
Lying on your back, palpate your breast with your fingertips. Wrap your fingers around your entire chest from top to bottom and side to side – from your collarbones to your upper abdomen and from your armpit to your cleavage. You should be able to feel down to the rib cage.
In the same way, check your breasts while sitting or standing with one hand raised above your head.
Worrying signs include any discharge from the nipple that is not related to breastfeeding.

In breast self-diagnosis, it is important to pay attention to any changes. If you notice any unusual symptoms, you should consult your doctor. There is no need to panic, as in most cases the lumps detected turn out to be benign.
Method 2. Mammography of the breast
The World Health Organisation recommends the use of mammography as the main screening method for breast cancer in women who are not at high risk of developing cancer.
Mammography of the breast is a method of looking for lumps using low-dose radiation. Mammography successfully diagnoses breast cancer in 78% of women under 50 and 83% of patients over 50. The method cannot show whether the abnormal area is cancerous or not; therefore, additional examinations must be carried out afterwards. Among every 1,000 women who have an annual mammogram, only 2-4 are diagnosed with cancer.
The dose of radiation that is given off during a mammogram is small and poses no danger to humans. On average, a modern mammographer emits around 0.4 mSv in one examination. By comparison, the average person receives 3 mSv in a year without any health risk.
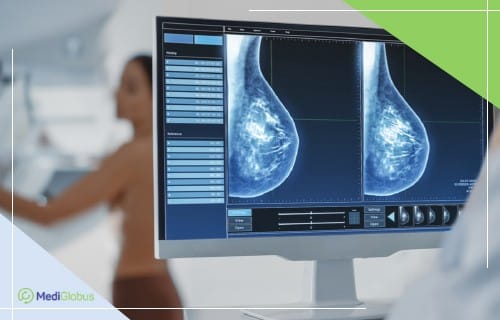
Sometimes women may be asked to have a second check-up after a mammogram. This does not mean that the doctors have detected cancer. A follow-up call after a screening mammogram is quite common. It often means that additional X-rays or an ultrasound scan is needed to examine the problem area in more detail. In 9 out of 10 patients who are invited for a second examination, no traces of cancer are detected.
Among the problems associated with mammography are false negatives and false positives. A false negative test does not detect a tumour, even if one is present. This problem is more common among women with dense breast tissue. In experienced cancer centres, this factor is taken into account during diagnosis and patients are referred for a breast ultrasound before a biopsy is ordered.
A falsely positive mammogram indicates cancer when in fact it does not exist. Most often, oncologists mistake ductal carcinoma in situ or benign tumours for cancer. This can lead to the prescription of unnecessary treatment. However, false positive diagnoses occur in only 1-10% of cases. It is more common to be misdiagnosed in:
Young women;
Patients with dense breast tissue;
Women who are at high risk of cancer;
Women taking oestrogen (e.g. oral contraceptives).
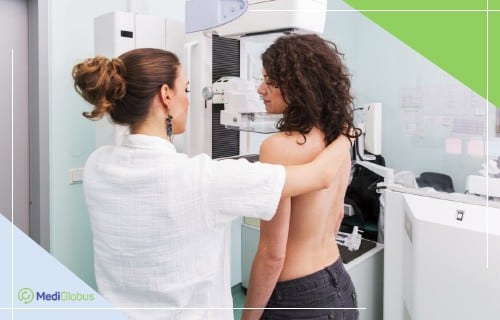
To reduce the risk of misdiagnosis, you should go to clinics that specialise in the treatment of breast cancer. Experienced radiologists working in these centres are more accurate in interpreting images.
Some foreign clinics use digital breast tomosynthesis, also known as 3D mammography, instead of standard mammography. This method reduces the likelihood of reapplying for a second examination and is indicated for women with dense breasts. The accuracy of tomosynthesis is 97,7%.
To find out which clinics abroad offer 3D mammography, write to our coordinating doctors. We can help you find a clinic and arrange a diagnosis at a time that is convenient for you.
Advice for women before an annual mammogram:
If you have had a breast augmentation, ask the clinic if they have experience of doing mammograms with implants. You will need 4 more scans than usual. These are called “implant displacement scans”.
Try not to have the examination in the week immediately before your period.
If you are likely to be pregnant, tell your radiologist. Although the risk to the foetus is very low and mammography is generally considered safe during pregnancy, the procedure is usually postponed until after you give birth.
Try to visit the same facility each time so that your mammograms can be easily compared from year to year. When you go to a new health centre, take the results of the previous year’s examinations with you.
MAMMOGRAPHY APPOINTMENT
Leave a request on our website and our coordinator will contact you shortly using the phone number you have provided. We will help you choose a clinic and doctor, organise your trip, arrange your documents, find an interpreter and deal with other organisational issues.
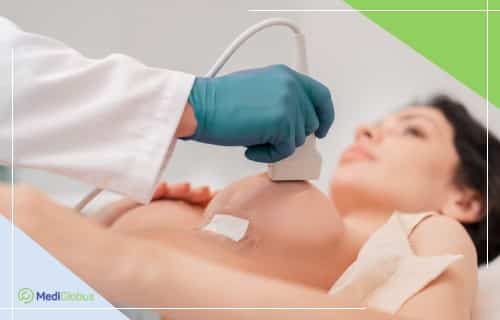
Method 3. Breast ultrasound
Ultrasound is used to diagnose neoplasms in women with dense breast tissue. The method is also used if there is a need to check an abnormal area that is not easily visible on a mammogram.
Ultrasound is useful in that it can often be used to distinguish between fluid-filled cysts and solid masses, which may require further examination.
Ultrasound is also used in biopsies to guide the needle to the tumour or enlarged lymph nodes.
Modern alternatives to breast ultrasound include Automated breast ultrasound (ABUS). This method uses a much larger sensor to take hundreds of images, covering almost the entire breast. The technology is approved by the FDA for screening women with dense breasts. Compared to conventional ultrasound, which has an accuracy rate of 91.4%, ABUS allows a correct diagnosis in 97,1% of cases.
Method 4. Thermography of the breast
Many websites recommend thermography as a safe and effective alternative to mammography in the diagnosis of breast cancer. It is a non-invasive method of examining heat patterns and blood flow on the surface of the body using an infra-red camera.
Although thermography is not harmful to the body in itself, using it for breast cancer screening is not recommended. In 2019, the US FDA, which is one of the world’s most authoritative sources for monitoring the safety of medical standards, issued a warning about the use of thermography for breast screening. Based on analysis of large amounts of data, they found that thermography was unable to detect early stages of breast cancer or other diseases, even in combination with other methods. Women who use this method of diagnosis instead of mammography or ultrasound run the risk of missing the disease at a vulnerable stage. Advertising of this method in the USA is considered to spread false information and is punishable by law.
Method 6. MRI of the breast

Magnetic resonance imaging (MRI) of the breast uses radio waves and strong magnets to take detailed pictures of the inside of the breast.
Breast imaging, together with mammography, is recommended by the FDA for screening women over the age of 30 with an increased risk of developing breast cancer.
The method is not used when screening most patients, as there is an increased risk of detecting false positive masses and appointing unnecessary biopsies.
Breast imaging also requires special equipment, which is not available in all hospitals. The machine is also used in MRI-guided breast biopsies.
The examination procedure is painless and usually takes 45-60 minutes. The images are processed quickly and the patient can receive a report within 1-2 hours of the examination.
Method 7. Molecular breast imaging
Molecular breast imaging (MBI), also known as scintimammography or breast specific gamma imaging (BSGI), is a type of breast investigation using nuclear medicine. A radioactive substance is injected into the bloodstream, the movement of which can be monitored using a special camera. The accumulation of the contrast agent usually indicates a focus of the cancer process. The results are indicative for patients with an average breast density as well as for those with a high breast density. This test is prescribed when the doctor detects an abnormality in a standard mammogram. The method is also used to determine the stage of already diagnosed cancer. Scintigraphy is not used for standard annual screening.
Method 8. Positron emission mammography (PET)
Positron emission mammography (PET) is a breast imaging method similar to a PET scan. A small amount of radioactive sugar is injected into the bloodstream to detect cancer cells. Its movement and accumulation is monitored on the machine. A few hours after the test the contrast is completely eliminated from the body with the urine.
A PET scan helps detect small clusters of cancer cells in the breast. The main purpose of using the PEM-test is breast cancer staging. The method is 70-97% accurate.
Method 9. CESM
Contrast-enhanced spectral mammography (CEM/CESM) is a modern technique that may soon replace MRI. It uses an iodine-containing dye that is injected into a vein a few minutes before two sets of mammograms are taken, using different energy levels. The contrast helps the X-rays show any abnormal areas in the breast. This test can be used to get a better look at areas that look abnormal on a standard mammogram, or to help estimate the size of a tumour in women with cancer. CEM is quicker and less expensive than an MRI scan.
Method 10. Elastography
Elastography is another new method for early diagnosis of breast cancer. It is based on an ultrasound examination of the compressed breast tissue. The test makes it possible to distinguish benign neoplasms (cysts) from cancerous ones. The latter appear on the image as denser and stiffer areas. Some clinical studies show that its effectiveness is comparable or higher than that of a standard ultrasound scan.
APPOINTMENT FOR A CONSULTATION
In addition to the quality of the equipment, the experience of the oncologist plays a major role in the correct diagnosis. MediGlobus can suggest the most professional breast cancer specialists who can conduct in-person and online consultations to clarify the diagnosis and recommendations for treatment. To get an international doctor’s opinion, leave an order form on our website.
Where do I go for breast screening?
The most suitable medical centres for quality breast examinations are multidisciplinary clinics with a strong oncology department. A large number of patients with different diseases visit them each year, so that the diagnosticians are experienced in distinguishing malignant from benign tumours.
You should also look at hospitals that work closely with universities. They often employ highly specialised specialists and have access to state-of-the-art equipment.
Among the leading medical centres that MediGlobus specialists can recommend are:
Breast check-up |
|---|
| Consultation with a specialist |
| Breast mammography/ultrasound/MRI |
| Cancer risk assessment |
| Blood test for cancer markers |
| Quick results and report |
Summary
Breast cancer detected in its early stages can be cured in 90-99% of cases. The most effective method of catching the disease in the period when it has no symptoms, is to have regular breast screening. Most women are advised to start screening at the age of 40-45. If there is a predisposition to cancer, check-ups should be done from the age of 30.
Most women only need a mammogram for reliable results. Some hospitals offer a 3D mammogram as a more advanced alternative.
Women who are at high risk of developing breast cancer are advised to have a mammogram together with a CT scan for early diagnosis.
If the doctor finds a suspicious mass on the scan, he or she will prescribe additional examinations. An ultrasound scan of the mammary glands is the most common examination, but scintigraphy, positron emission mammography, contrast-enhanced mammography and elastography are also used.
MediGlobus recommends breast screening at the following clinics: Medical Park Antalya, Hisar, Chaim Shiba Medical Center, University Hospital of Cologne, Vienna Private Hospital, University Hospital of Navarra.
MediGlobus coordinating doctors provide free assistance in arranging diagnosis and treatment of illnesses abroad. Leave your application online by clicking on the button below and we will help you get a quick response from the clinic you are interested in.
Sources:
- 1. American Association of Oncologists
- 2. FDA warning on thermography
- 3. Egyptian Journal of Radiology and Nuclear Medicine
- 4.UCHealth about mammography
- 6. Scientific reports
- 7. Applied Radiology
- 8. Ultrasonography